17 Apr Five Things You Can Do to Improve Time in Range
(But Remember, It’s Not Always Perfect)
Living with Type 1 Diabetes (T1D) is a constant balancing act. You’re counting carbs, adjusting insulin doses, and sticking to a routine—but sometimes, despite your best efforts, your blood glucose (BG) still refuses to stay within range. If you’ve ever had those frustrating days when your BG seems all over the place, even when you feel like you’re doing everything right, you’re not alone. It’s important to remember that diabetes management isn’t always linear, and there’s a lot of unpredictability built into the process.
That said, let’s talk about how you can improve your time in range (TIR) without making it sound like an unreachable goal. Small changes can make a big difference, but it’s also okay to give yourself grace when things don’t go as planned.
I’m Megan, Ellie’s mom, and I’m pinch hitting (okay, posting) for Ellie while she is immersed in test prep (International Baccalaureate exams, ACT, end of course or EOC, etc.). I help Ellie, attend her endo appointments, and learn as we go. We’re sharing five tips that could help you improve your time in range—and yes, while it may not always be perfect, these steps can set you on a path toward a more consistent BG.
1
Tighten Up Your Carb Counting—But Don’t Stress the Small Stuff
Carb counting is one of the cornerstones of diabetes management, and getting a solid grip on it can significantly improve your BG control. But here’s the thing: No one’s going to get it perfectly every single time, and that’s okay. It’s not about being 100% accurate down to the gram (unless you’re really into precision). Instead, focus on being consistent and creating a pattern that works for you. Use food scales or apps that track your carb intake to help. But, also be gentle with yourself when things aren’t exactly as planned. A little wiggle room can still lead to big results.
2
Consider Your Insulin to Carb Ratio—And Adjust When Needed
You’ve probably heard this one a lot, but it’s true: Insulin-to-carb ratios (ICR) aren’t set in stone. They can change depending on the time of day, how active you are, or even how much stress you’re under. The good news is that you can tweak this ratio. Some people notice that their insulin needs are slightly different for breakfast compared to dinner, or that after a workout, they need less insulin for the same meal. The more you fine-tune your ICR based on patterns you notice, the more your TIR might improve. We do this in consultation with Ellie’s diabetes team at Children’s Mercy Kansas City. Her ratios are stored in her insulin pump so that it calculates the amount of insulin based on the number of carbs she enters into the pump. She has three different ratios throughout the day.
3
Don’t Underestimate the Power of Routine (Even When It Feels Like a Snooze)
A solid routine—sleeping at the same time, eating at consistent hours, and taking your insulin in a regular pattern—can be a game changer for maintaining stable BG levels. We get it, though: Life is chaotic, and routines aren’t always easy to stick to. But, consistency can work wonders. When you keep your schedule as predictable as possible, your body tends to respond better to insulin, and your BG will have fewer wild swings. That doesn’t mean everything will be perfect every day (spoiler alert: it won’t be), but it can give you a better shot at those more stable days. Right now, we’re grateful for the August-May school day routine of getting up, eating, exercising, and going to bed at roughly the same time each day.
4
Incorporate Exercise Regularly (But, Watch Out for the Post-Exercise Drop)
Exercise is one of those things that can help lower your blood sugar and improve insulin sensitivity. But it’s not always straightforward—sometimes you might find yourself riding a rollercoaster of highs and lows after a workout. For Ellie, regular exercise helps stabilize her BG in the long term, but we’re mindful of how it affects her insulin needs, especially if she’s doing intense workouts or exercising over an extended period (walking/hiking). If you’re heading into a run or strength training, check your BG beforehand and make necessary adjustments to prevent a post-exercise crash. About an hour before exercise, Ellie puts her insulin pump in “activity” mode to elevate her target BG from 110 to 150, and she always carries fast acting carbs. The key is consistency, so make movement part of your routine but monitor your BG closely in the hours afterward.
5
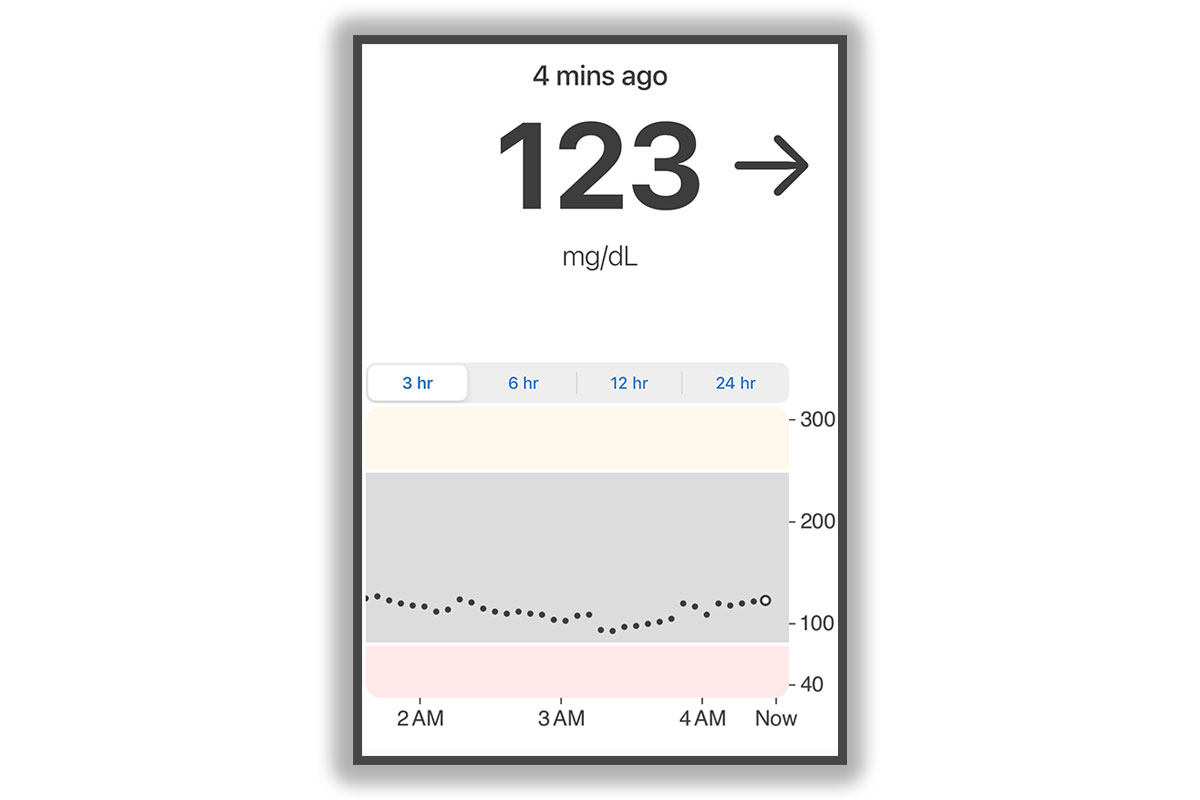
Stay on Top of Continuous Glucose Monitoring (CGM) Data (And Don’t Freak Out Over the Ups and Downs)
If you’re lucky enough to have a CGM, you know how helpful it is to have real-time data on your BG. However, that also means you’re probably seeing a lot of fluctuations throughout the day. It’s totally normal for BG levels to go up and down—even with a perfectly calculated meal or perfect insulin dose. The beauty of a CGM is that you can see the trends and make adjustments as needed. If your CGM is showing a bit more of a rollercoaster than you’d like, don’t panic. Look at the patterns over time, not just the individual blips. Sometimes your body just needs a little extra time to find its rhythm, even if your management plan is rock solid. We try to think of BG readings as data points, not grades. Your BG is info on which you base decisions (not a grade).
The Truth: It’s Not Always Smooth Sailing
While these five tips can help improve your time in range, it’s crucial to remember that managing T1D isn’t about chasing perfection. BGs can be all over the place, even when you’re doing everything right. Stress, illness, hormonal changes, etc. can impact how your body responds to insulin. It’s all part of the journey.
So, don’t beat yourself up over every high or low. Celebrate the small victories and know that it’s okay to have those days when things don’t go according to plan. The most important thing is that you’re doing your best, and that’s more than enough.
At The Helpful Type, we believe in giving ourselves—and each other—some grace in this unpredictable adventure that is type one diabetes. You’ve got this!
If you found this post helpful, feel free to share it with a friend or leave a comment below with your own tips or experiences. We’d love to hear from you!



